Fast and efficient isolation of murine circulating tumor cells using screencell technology for pre-clinical analyzes
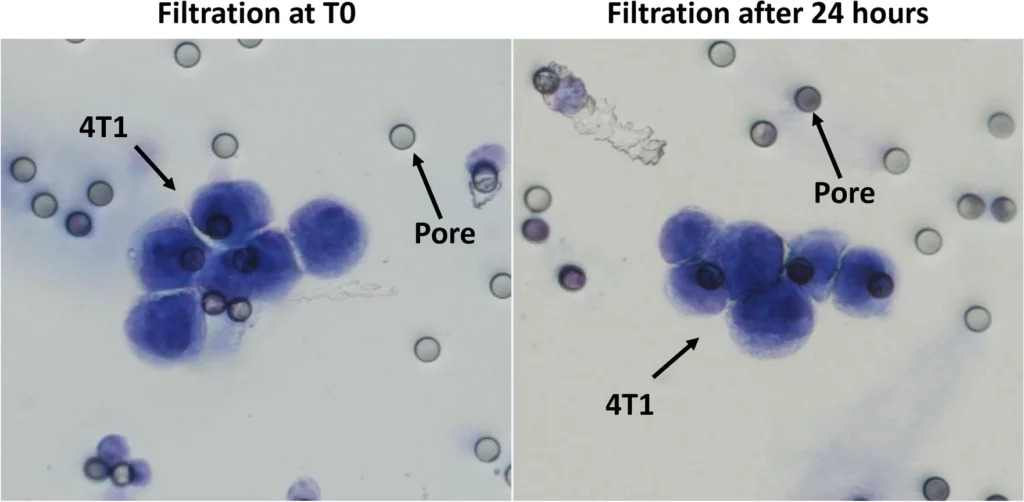
Circulating tumor cells (CTCs) represent a rare and heterogeneous population of cancer cells that are detached from the tumor site and entered blood or lymphatic circulation. Once disseminated in distant tissues, CTCs could remain dormant or create a tumor mass causing serious danger for patients. Many technologies exist to isolate CTCs from patients’ blood samples, mostly based on microfluidic systems or by sorting them according to their surface antigens, notably EpCAM, and/or cytokeratins for carcinoma. ScreenCell has developed an easy-to-use, antigen-independent, rapid, cost-effective, and efficient technology that isolates CTCs according to their bigger size compared to the blood cells. This study provides the technical information necessary to isolate and characterize CTCs from mouse blood. By using blood samples from transgenic mice with breast cancer or from WT mice in which we spiked cancer cells, we showed that ScreenCell technology is compatible with standard EDTA blood collection tubes. Furthermore, the ScreenCell Cyto kit could treat up to 500 µl and the ScreenCell MB kit up to 200 µl of mouse blood. As the ScreenCell MB kit captures unaltered live CTCs, we have shown that their DNA could be efficiently extracted, and the isolated cells could be grown in culture. In conclusion, ScreenCell provides a rapid, easy, antigen-independent, cost-effective, and efficient technology to isolate and characterize CTCs from the blood samples of cancer patients and murine models. Thanks to this technology CTCs could be captured fixed or alive. Murine cancer models are extensively used in pre-clinical studies. Therefore, this study demonstrates the crucial technical points necessary while manipulating mouse blood samples using ScreenCell technology.
Gene signatures of circulating breast cancer cell models are a source of novel molecular determinants of metastasis and improve circulating tumor cell detection in patients
Background: Progression to stage IV disease remains the main cause of breast cancer-related deaths. Increasing knowledge on the hematogenous phase of metastasis is key for exploiting the entire window of opportunity to interfere with early dissemination and to achieve a more effective disease control. Recent evidence suggests that circulating tumor cells (CTCs) possess diverse adaptive mechanisms to survive in blood and eventually metastasize, encouraging research into CTC-directed therapies.
Methods: On the hypothesis that the distinguishing molecular features of CTCs reveal useful information on metastasis biology and disease outcome, we compared the transcriptome of CTCs, primary tumors, lymph-node and lung metastases of the MDA-MB-231 xenograft model, and assessed the biological role of a panel of selected genes, by in vitro and in vivo functional assays, and their clinical significance in M0 and M+ breast cancer patients.
Results: We found that hematogenous dissemination is governed by a transcriptional program and identified a CTC signature that includes 192 up-regulated genes, mainly related to cell plasticity and adaptation, and 282 down-regulated genes, involved in chromatin remodeling and transcription. Among genes up-regulated in CTCs, FADS3 was found to increases cell membrane fluidity and promote hematogenous diffusion and lung metastasis formation. TFF3 was observed to be associated with a subset of CTCs with epithelial-like features in the experimental model and in a cohort of 44 breast cancer patients, and to play a role in cell migration, invasion and blood-borne dissemination. The analysis of clinical samples with a panel of CTC-specific genes (ADPRHL1, ELF3, FCF1, TFF1 and TFF3) considerably improved CTC detection as compared with epithelial and tumor-associated markers both in M0 and stage IV patients, and CTC kinetics informed disease relapse in the neoadjuvant setting.
Conclusions: Our findings provide evidence on the potential of a CTC-specific molecular profile as source of metastasis-relevant genes in breast cancer experimental models and in patients. Thanks to transcriptome analysis we generated a novel CTC signature in the MDA-MB-231 xenograft model, adding a new piece to the current knowledge on the key players that orchestrate tumor cell hematogenous dissemination and breast cancer metastasis, and expanding the list of CTC-related biomarkers for future validation studies.
Identification of Atypical Circulating Tumor Cells with Prognostic Value in Metastatic Breast Cancer Patients

Circulating tumor cells have a strong potential as a quasi-non-invasive tool for setting up a precision medicine strategy for cancer patients. Using a second-generation « filtration-based » technology to isolate CTCs, the Screencell™ technology (Sarcelles, France), we performed a large and simultaneous analysis of all atypical circulating tumor cells (aCTCs) isolated from the blood of metastatic breast cancer (mBC) patients. We correlated their presence with clinicopathological and survival data. We included 91 mBC patients from the PERMED-01 study. The median number of aCTCs was 8.3 per mL of blood. Three subsets of aCTCs, absent from controls, were observed in patients: single (s-aCTCs), circulating tumor micro-emboli (CTM), and giant-aCTCs (g-aCTCs). The presence of g-aCTCs was associated with shorter progression free survival and overall survival. This study highlights the heterogeneity of aCTCs in mBC patients both at the cytomorphological and molecular levels. In addition, it suggests the usefulness of the g-aCTC subset as a prognostic factor and a potential stratification tool to treat late-stage mBC patients and improve their chances of benefiting from early clinical trials.
Circulating Tumor Cell Clusters Are Frequently Detected in Women with Early-Stage Breast Cancer

The clinical relevance of circulating tumor cell clusters (CTC-clusters) in breast cancer (BC) has been mostly studied using the CellSearch®, a marker-dependent method detecting only epithelial-enriched clusters. However, due to epithelial-to-mesenchymal transition, resorting to marker-independent approaches can improve CTC-cluster detection. Blood samples collected from healthy donors and spiked-in with tumor mammospheres, or from BC patients, were processed for CTC-cluster detection with 3 technologies: CellSearch®, CellSieve™ filters, and ScreenCell® filters. In spiked-in samples, the 3 technologies showed similar recovery capability, whereas, in 19 clinical samples processed in parallel with CellSearch® and CellSieve™ filters, filtration allowed us to detect more CTC-clusters than CellSearch® (median number = 7 versus 1, p = 0.0038). Next, samples from 37 early BC (EBC) and 23 metastatic BC (MBC) patients were processed using ScreenCell® filters for attaining both unbiased enrichment and marker-independent identification (based on cytomorphological criteria). At baseline, CTC-clusters were detected in 70% of EBC cases and in 20% of MBC patients (median number = 2, range 0-20, versus 0, range 0-15, p = 0.0015). Marker-independent approaches for CTC-cluster assessment improve detection and show that CTC-clusters are more frequent in EBC than in MBC patients, a novel finding suggesting that dissemination of CTC-clusters is an early event in BC natural history.
Immunomodulatory Activity of a Colony-stimulating Factor-1 Receptor Inhibitor in Patients with Advanced Refractory Breast or Prostate Cancer: A Phase I Study.

Purpose: Tumor-associated macrophages correlate with increased invasiveness, growth, and immunosuppression. Activation of the colony-stimulating factor-1 receptor (CSF-1R) results in proliferation, differentiation, and migration of monocytes/macrophages. This phase I study evaluated the immunologic and clinical activity, and safety profile of CSF-1R inhibition with the mAb LY3022855.
Patients and methods: Patients with advanced refractory metastatic breast cancer (MBC) or metastatic castration-resistant prostate cancer (mCRPC) were treated with LY3022855 intravenously in 6-week cycles in cohorts: (A) 1.25 mg/kg every 2 weeks (Q2W); (B) 1.0 mg/kg on weeks 1, 2, 4, and 5; (C) 100 mg once weekly; (D)100 mg Q2W. mCRPC patients were enrolled in cohorts A and B; patients with MBC were enrolled in all cohorts. Efficacy was assessed by RECIST and Prostate Cancer Clinical Trials Working Group 2 criteria.
Results: Thirty-four patients (22 MBC; 12 mCRPC) received ≥1 dose of LY3022855. At day 8, circulating CSF-1 levels increased and proinflammatory monocytes CD14DIMCD16BRIGHT decreased. Best RECIST response was stable disease in five patients with MBC (23%; duration, 82-302 days) and three patients with mCRPC (25%; duration, 50-124 days). Two patients with MBC (cohort A) had durable stable disease >9 months and a third patient with MBC had palpable reduction in a nontarget neck mass. Immune-related gene activation in tumor biopsies posttreatment was observed. Common any grade treatment-related adverse events were fatigue, decreased appetite, nausea, asymptomatic increased lipase, and creatine phosphokinase.
Conclusions: LY3022855 was well tolerated and showed evidence of immune modulation. Clinically meaningful stable disease >9 months was observed in two patients with MBC.
Circulating tumour cell enumeration does not correlate with Miller-Payne grade in a cohort of breast cancer patients undergoing neoadjuvant chemotherapy

Purpose: The association between pathological complete response (pCR) in patients receiving neoadjuvant chemotherapy (NAC) for breast cancer and Circulating Tumour Cells (CTCs) is not clear. The aim of this study was to assess whether CTC enumeration could be used to predict pathological response to NAC in breast cancer as measured by the Miller-Payne grading system.
Methods: Twenty-six patients were recruited, and blood samples were taken pre- and post-NAC. CTCs were isolated using the ScreenCell device and stained using a modified Giemsa stain. CTCs were enumerated by 2 pathologists and classified as single CTCs, doublets, clusters/microemboli and correlated with the pathological response as measured by the Miller-Payne grading system. χ2 or ANOVA was performed in SPSS 24.0 statistics software for associations.
Results: 89% of patients had invasive ductal carcinoma (IDC) and 11% invasive lobular carcinoma (ILC). At baseline 85% of patients had CTCs present, median 7 (0-161) CTCs per 3 ml of whole blood. Post-chemotherapy, 58% had an increase in CTCs. This did not correlate with the Miller-Payne grade of response. No significant association was identified between the number of CTCs and clinical characteristics; however, we did observe a correlation between pre-treatment CTC counts and body mass index, p < 0.05. Conclusions: Patients with a complete response to NAC still had CTCs present, suggesting enumeration is not sufficient to aid surgery stratification. Additional characterisation and larger studies are needed to further characterise CTCs isolated pre- and post-chemotherapy. Long-term follow-up of these patients will determine the significance of CTCs in NAC breast cancer patients.
Comparative performance of different methods for circulating tumor cell enrichment in metastatic breast cancer patients

The isolation and analysis of circulating tumor cells (CTC) has the potential to provide minimally invasive diagnostic, prognostic and predictive information. Widespread clinical implementation of CTC analysis has been hampered by a lack of comparative investigation between different analytic methodologies in clinically relevant settings. The objective of this study was to evaluate four different CTC isolation techniques-those that rely on surface antigen expression (EpCAM or CD45 using DynaBeads® or EasySep™ systems) or the biophysical properties (RosetteSep™ or ScreenCell®) of CTCs. These were evaluated using cultured cells in order to calculate isolation efficiency at various levels including; inter-assay and inter-operator variability, protocol complexity and turn-around time. All four techniques were adequate at levels above 100 cells/mL which is commonly used for the evaluation of new isolation techniques. Only the RosetteSep™ and ScreenCell® techniques were found to provide adequate sensitivity at a level of 10 cells/mL. These techniques were then applied to the isolation and analysis of circulating tumor cells blood drawn from metastatic breast cancer patients where CTCs were detected in 54% (15/28) of MBC patients using the RosetteSep™ and 75% (6/8) with ScreenCell®. Overall, the ScreenCell® method had better sensitivity.
Rapid and Sensitive Detection of Breast Cancer Cells in Patient Blood with Nuclease-Activated Probe Technology

A challenge for circulating tumor cell (CTC)-based diagnostics is the development of simple and inexpensive methods that reliably detect the diverse cells that make up CTCs. CTC-derived nucleases are one category of proteins that could be exploited to meet this challenge. Advantages of nucleases as CTC biomarkers include: (1) their elevated expression in many cancer cells, including cells implicated in metastasis that have undergone epithelial-to-mesenchymal transition; and (2) their enzymatic activity, which can be exploited for signal amplification in detection methods. Here, we describe a diagnostic assay based on quenched fluorescent nucleic acid probes that detect breast cancer CTCs via their nuclease activity. This assay exhibited robust performance in distinguishing breast cancer patients from healthy controls, and it is rapid, inexpensive, and easy to implement in most clinical labs. Given its broad applicability, this technology has the potential to have a substantive impact on the diagnosis and treatment of many cancers.
Detection and Characterization of Circulating Tumor Associated Cells in Metastatic Breast Cancer

The availability of blood-based diagnostic testing using a non-invasive technique holds promise for real-time monitoring of disease progression and treatment selection. Circulating tumor cells (CTCs) have been used as a prognostic biomarker for the metastatic breast cancer (MBC). The molecular characterization of CTCs is fundamental to the phenotypic identification of malignant cells and description of the relevant genetic alterations that may change according to disease progression and therapy resistance. However, the molecular characterization of CTCs remains a challenge because of the rarity and heterogeneity of CTCs and technological difficulties in the enrichment, isolation and molecular characterization of CTCs. In this pilot study, we evaluated circulating tumor associated cells in one blood draw by size exclusion technology and cytological analysis. Among 30 prospectively enrolled MBC patients, CTCs, circulating tumor cell clusters (CTC clusters), CTCs of epithelial-mesenchymal transition (EMT) and cancer associated macrophage-like cells (CAMLs) were detected and analyzed. For molecular characterization of CTCs, size-exclusion method for CTC enrichment was tested in combination with DEPArray™ technology, which allows the recovery of single CTCs or pools of CTCs as a pure CTC sample for mutation analysis. Genomic mutations of TP53 and ESR1 were analyzed by targeted sequencing on isolated 7 CTCs from a patient with MBC. The results of genomic analysis showed heterozygous TP53 R248W mutation from one single CTC and pools of three CTCs, and homozygous TP53 R248W mutation from one single CTC and pools of two CTCs. Wild-type ESR1 was detected in the same isolated CTCs. The results of this study reveal that size-exclusion method can be used to enrich and identify circulating tumor associated cells, and enriched CTCs were characterized for genetic alterations in MBC patients, respectively.
Did circulating tumor cells tell us all they could? The missed circulating tumor cell message in breast cancer

Purpose: To compare circulating tumor cell (CTC) detection rates in patients with early (M0) and metastatic (M+) breast cancer using 2 positive-selection methods or size-based unbiased enrichment.
Methods: Blood collected at baseline and at different times during treatment from M0 patients undergoing neoadjuvant therapy and from M+ women starting a new line of treatment was processed in parallel using AdnaTest EMT-1/ and EMT-2/Stem CellSelect/Detect kits or ScreenCell Cyto devices. CTC positivity was defined according to the suggested cutoffs and cytological parameters, respectively.
Results: Higher CTC detection rates were obtained with the AdnaTest approach when using for CTC-enrichment antibodies against ERBB2 and EGFR in addition to MUC1 and the classical epithelial surface marker EPCAM (13% vs. 48%). In M0 patients mainly, CTC positivity rates further increased when EMT- and stemness-related marker expression (PIK3CA, AKT2 and ALDH1) was evaluated in addition to EPCAM, MUC1 and ERBB2. When the physical properties of tumor cells were exploited, CTCs were detected at higher percentages than with positive-selection-based methods, without any difference between clinical stages (78% in M0 vs. 72% in M+ cases at baseline). Circulating tumor microemboli (CTMs) were detected in addition to single CTCs with significantly higher frequency in M0 than M+ samples (78% vs. 27%, p = 0.0002).
Conclusions: Different approaches for CTC detection probably identify distinct tumor cell subpopulations, but need technical standardization before their clinical validity and biological specificity may be adequately investigated. The distinct role of CTMs compared with CTCs as prognostic and predictive biomarkers represents a further challenge.